This website uses cookies so that we can provide you with the best user experience possible. Cookie information is stored in your browser and performs functions such as recognising you when you return to our website and helping our team to understand which sections of the website you find most interesting and useful.
What is Haemophilia?
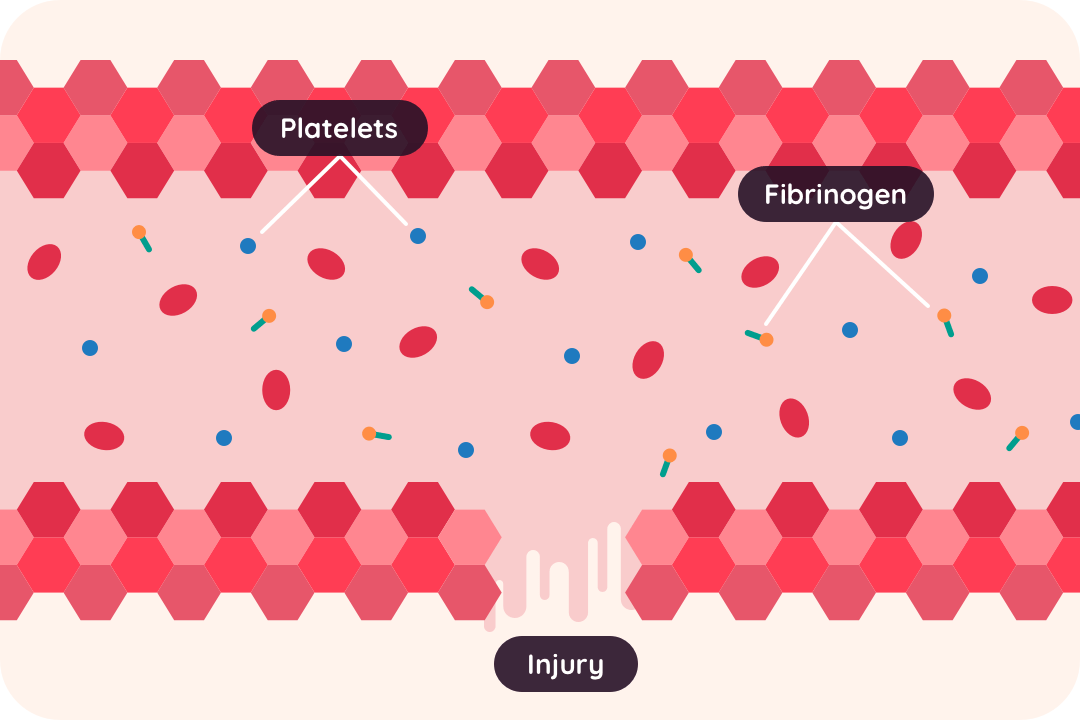
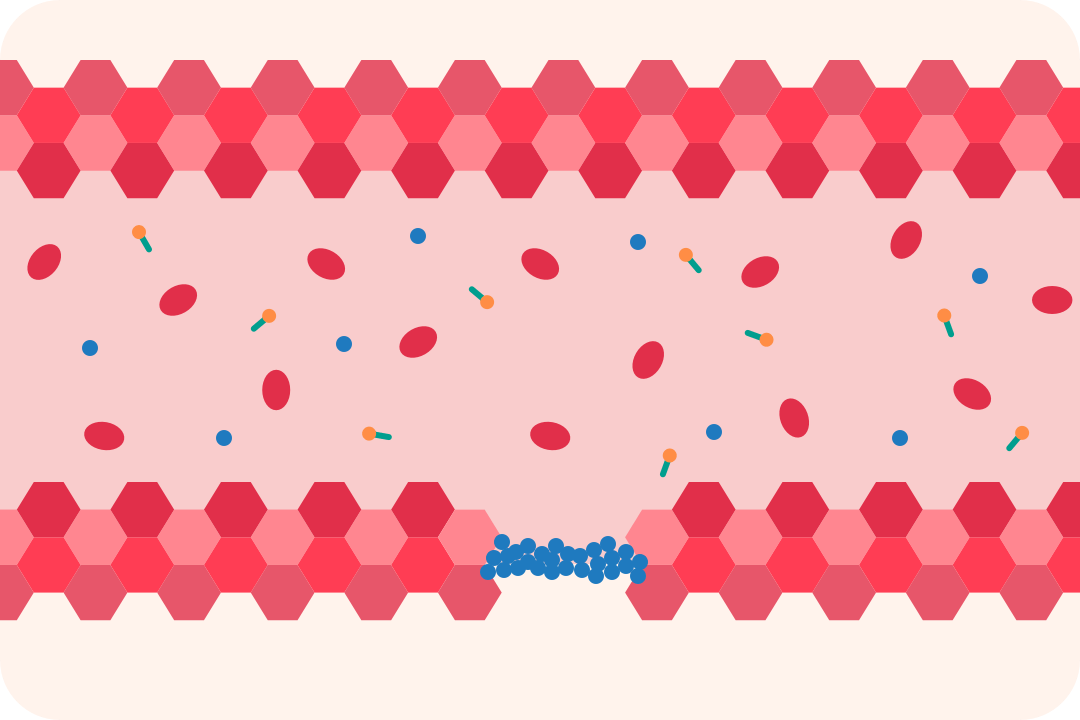
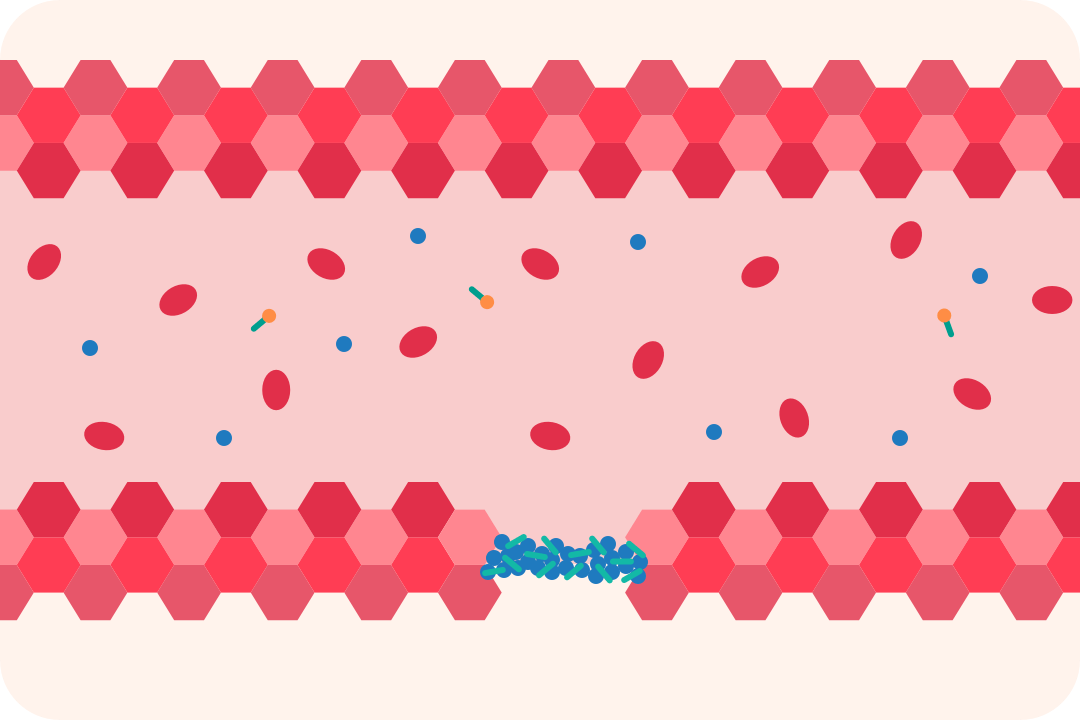
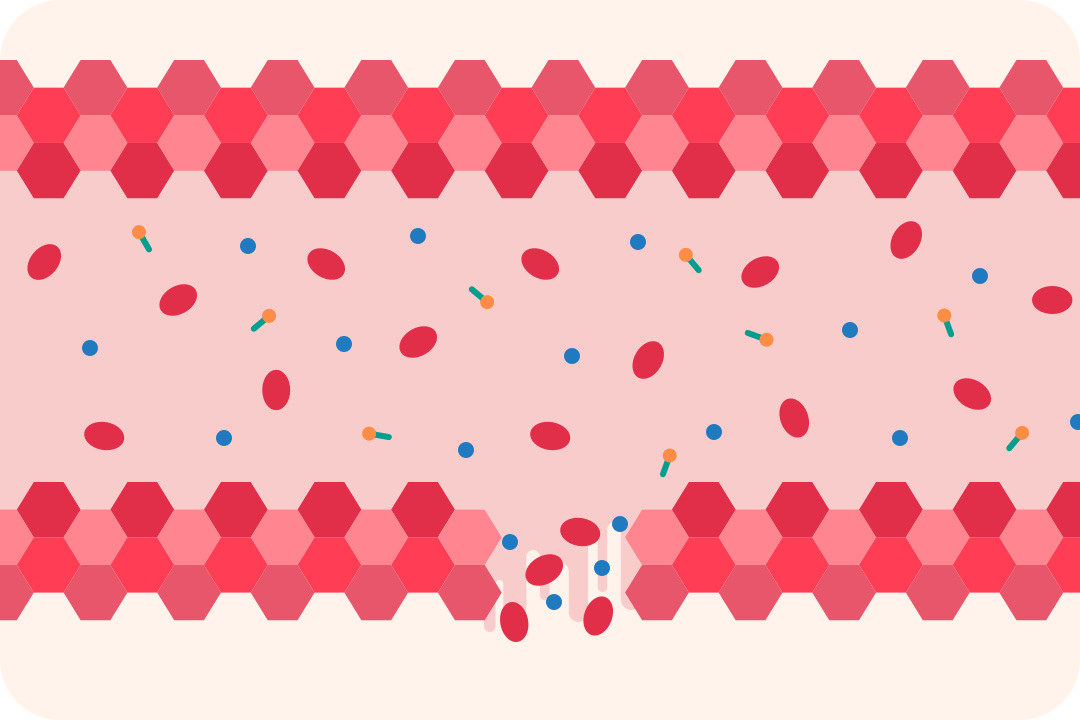
Haemophilia is a rare medical condition that affects the blood's ability to clot. It's usually inherited, although one in three babies born with haemophilia will have no known family history of it. Most people who have haemophilia are male.
1 in 10,000
males in the UK are
affected by Haemophilia
fewer than 1,000
females in the UK have
Haemophilia